CERVICAL SCREENING (PAP/SMEAR) TEST
The NHS cervical screening programme is available to women aged 25 to 64 in England. All eligible women who are registered with a GP automatically receive an invitation by mail. Women aged 25 to 49 receive invitations every 3 years. Women aged 50 to 64 receive invitations every 5 years.
OVERVIEW
The tests used to screen women for cervical ‘pre-cancer’ are:
- The Papanicolaou or “Pap” test (sometimes called a “Pap smear”)
- The human papillomavirus or “HPV” test
The screening tests can detect cervical pre-cancer and even cancer in the early stages when it can be treated and thus aims to reduce the number of deaths from cervical cancer.
- The process is not perfect and in every screening programme there are a number of false positives and false negatives.
The NHS cervical screening programme is available to women aged 25 to 64 in England. All eligible women who are registered with a GP automatically receive an invitation by mail. Women aged 25 to 49 receive invitations every 3 years. Women aged 50 to 64 receive invitations every 5 years.
Some women choose to have the pap smear test more often (e.g. annually) and will need to make separate arrangements to facilitate this. This is sometimes performed as part of an annual ‘well-woman’ health check.
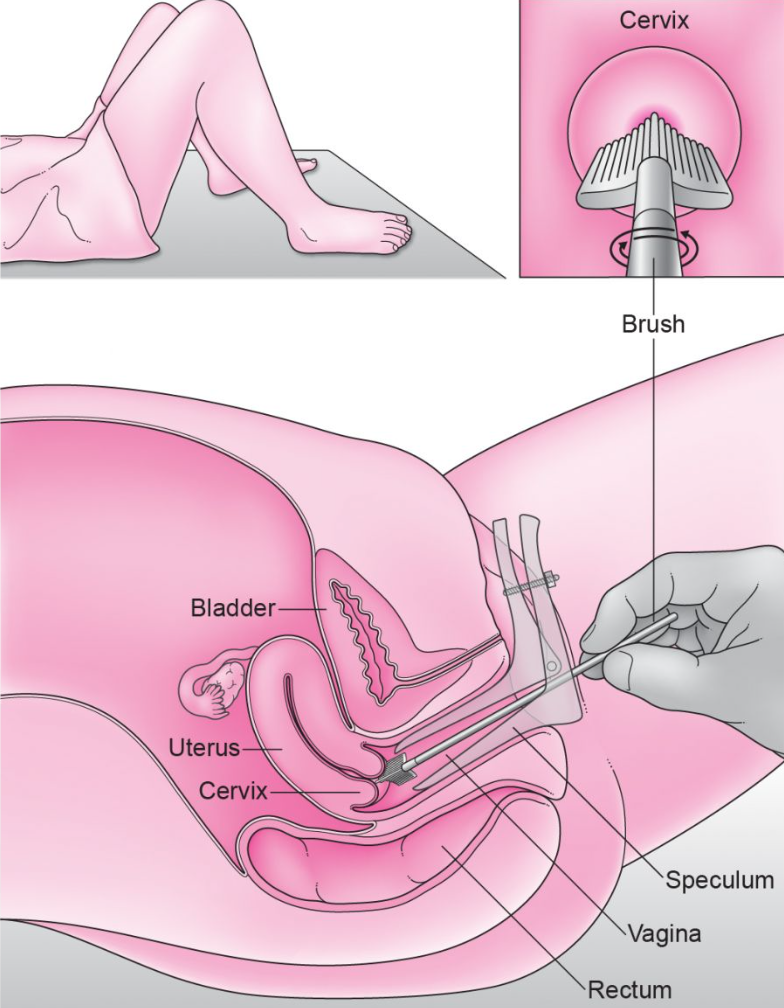
Cervical (Pap) smear
CERVICAL CANCER RISK FACTORS
The most important risk factor for cervical cancer is infection with the human papillomavirus (HPV). There are over 100 different types of HPV; however, most types of HPV do not cause cancer. At least 80 percent of women are exposed to the HPV virus during their lifetime. Most of the time the body’s immune system suppresses or gets rid of the virus before it does harm.
Researchers have labelled the HPV types as being high or low risk for causing cervical cancer.
- Low-risk HPV types – HPV types 6 and 11 can cause genital warts and are low-risk types because they rarely cause cervical cancer.
- High-risk HPV types – These may cause cervical cancer in some women. Although most women who are infected with the high-risk HPV types do not develop cervical cancer, women who test positive for high-risk HPV over many years are at a higher risk of cervical cancer. HPV types 16 and 18 are two of the high-risk types.
HPV is spread by direct skin-to-skin contact, including sexual intercourse or any other contact involving the genital area. It is not possible to become infected with HPV by touching an object, such as a toilet seat. Most people who are infected with HPV have no signs or symptoms. Most HPV infections are temporary and resolve within two years. When the virus persists (in 10 to 20 percent of cases), there is a chance of developing cervical pre-cancer or cancer. However, it usually takes many years for HPV infection to cause cervical cancer.
Since HPV is transmitted by sexual contact, having multiple sexual partners is associated with an increased risk for cervical cancer. Condoms provide only partial protection. Smoking can increase the risk of cervical cancer up to fourfold, as does having a condition or taking a medicine that weakens the immune system.
A vaccine to help prevent infection with some high-risk types of HPV is available. All girls can get the HPV vaccine free from the NHS from the age of 12 up to their 18th birthday. It helps protect them against cervical cancer, which is the most common cancer in women under 35 in the UK. In England, girls aged 12 to 13 years are routinely offered the first HPV vaccination when they’re in school year 8. The second dose is normally offered 6 to 12 months after the first (in school year 8 or year 9).
CERVICAL CANCER SCREENING TESTS
There are several ways to screen for cervical cancer. The traditional screening test is called a “Pap smear test.”
- This test is a method of examining cells from the neck of the womb (cervix).
- To perform a Pap smear test, a doctor or nurse will perform a pelvic exam and use a small brush to collect cells from the cervix.
- The cells are added to a preservative fluid (called liquid-based, thin layer testing).
HPV test — A human papillomavirus (HPV) test can be done along with a Pap smear test or as a separate test. Like a Pap smear test, the HPV test is done during a pelvic exam, using a small brush to collect a sample from the cervix. HPV tests do not test for all different types of HPV. They test for the strains of HPV that are the highest risk for causing cervical cancer.
Note: The role/timing of HPV testing is somewhat contentious. Various experts have recommended one of the following options:
- HPV primary screening – In this method the sample of cells taken during cervical screening is tested for HPV first. If ‘high risk’ HPV is found, cervical screening cytology (examination of the cells under a microscope) is then done to confirm if cell changes are present.
- HPV triage – For this method, cervical screening cytology is done first and if this shows a result of low grade abnormalities, HPV testing will then be carried out. If the test comes back positive for ‘high risk’ HPV the woman will be referred to colposcopy (procedure to look more closely at the cervix). If it is negative she will be returned to routine screening every three or five years
- Routine HPV testing with every Pap Smear test – The National Cancer Institute in the USA states the following: ‘For women aged 30 and older, Pap and HPV co-testing is less likely to miss an abnormality (i.e., has a lower false-negative rate) than Pap testing alone. Therefore, a woman with a negative HPV test and normal Pap test has very little risk of a serious abnormality developing over the next several years’.
